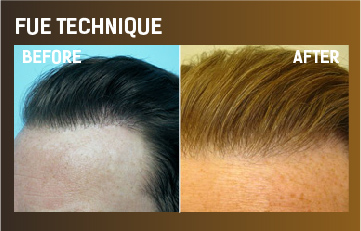
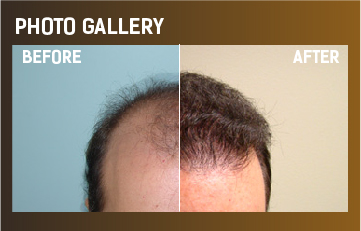
Hair loss in women is totally different than men and requires a very different approach. Here are some of the key gender differences regarding Hair Loss:
• 95%-98% of the hair loss men experience is Male Pattern Hair Loss [MPHL] vs. 40-60% of hair loss cases in women is actually Female Pattern of Hair Loss [FPHL], or androgenetic alopecia.
• Males primarily have defined hair loss patterns while females show decreased hair density diffusely at the top or sides of the scalp.
• Women also experience varying patterns of loss, occasionally resulting from chemical over processing and or certain styling techniques [i.e. tight braiding] that can actually result in traction alopecia.
• Hair loss in females may be even more devastating than in males.
• 70% of women vs. 25% of men expressed high levels of distress as a result of their hair loss.
• Ludwig Classification is used to evaluate hair loss in women
• Graying or balding in women is not perceived as “distinguished” as it is often seen in men. The usual assumption for female hair loss is aging or disease.

Each hair on the human scalp is unique and has a normal hair growth cycle. While hair growth cycle dynamics vary somewhat between different mammalian species and their location on the body, there are systemic and local factors that can modulate the hair follicle activity. The scalp hair growth cycle includes three phases: growth or anagen (2 to 8 years). The second phase, catagen (2-3 weeks) is transitional. The third phase is the resting (telogen) or shedding phase that last 3-4 months. This hair cycle is asynchronous. The scalp hair follicles are 86-89% in growth phase, 1% in transitional phase and 10-13% in the shedding phase. The hair growth rate is 0.3-0.5 mm/day or 1.0 – 1.5 cms/month. Generally speaking, we lose between 50-150 hairs everyday as part of a healthy shedding process. In most of the cases the hair regrows because the follicle is healthy and begins the anagen phase once again.

Hair loss in women can also be androgenetic, but not all clinically similar cases will have an androgen abnormality. Where no hyperandrogenemia can be shown, a diagnosis of telogen effluvium (hair shedding) or female pattern alopecia is more appropriate. The thinning [or FPHL] begins ages 12 and 40 years, Inheritance pattern is polygenic. In susceptible hair follicles, dihydrotestosterone binds to androgen receptors, and the hormone-receptor complex activates the genes responsible for the gradual transformation of large terminal follicles to miniaturized follicles.
The miniaturized follicles produce shorter and finer hairs of various lengths and diameters and these miniaturized hairs are the hallmark of the condition. In women, hair thinning, a diffusion of the scalp, is most marked on the frontal and parietal [sides] of the scalp. Women typically retain a rim of hair along the frontal hairline. Increased spacing between hairs makes the central part look wider over the frontal scalp compared to the occipital scalp. Overall, pattern hair loss in women is characterized by a more diffuse reduction in hair density than in men and this occurs principally over the top and frontal areas of the scalp.
Most women with FPHL have normal menses/pregnancies. Extensive hormonal testing may not be needed unless symptoms and signs of androgen excess are present, such as hirsutism, severe unresponsive cystic acne, virilization, or galactorrhea. While loss of scalp hair occurs in female hyperandrogenism, many exhibiting FPHL present with no clinical or biochemical evidence of androgen excess. Thus, the emerging view is that FPHL is likely to be a multifactorial, though genetically determined, trait with both androgen-dependent and androgen-independent mechanisms involved. Approximately 40-60% of women with hair loss are not FPHL related so other causes of hair loss should be ruled out.
Also important to note is that women often require more listening from their hair restoration physician versus talking during the consultation, as the physician needs to be keenly aware of their needs.
Classification for Hair Loss in Women
Ludwig has classified three different patterns of female pattern hair loss (see illustration below). Although the density of hair in a given pattern of loss tends to diminish with age, there is no way to predict what pattern of hair loss a woman with early FPHL will eventually assume. Some female patterns of hair loss can’t be found on the Ludwig classification scale. The classification is a good reference for an organized and systemic approach (medical and/or surgical) for the hair loss patient.

Other Causes of Hair Loss in Women
Hair loss clinically may be broadly grouped in several ways, the first of which is scarring vs. non-scarring alopecias. Clinically, non-scarring alopecias – the prototype of which is androgenetic alopecia or FPHL and alopecia areata – demonstrate hair loss without changes in the texture or appearance of the scalp. In general, scarring alopecias – the prototypes being lichen plano pilaris – on the other hand typically demonstrate associated changes of the skin (redness, inflammation, scabs, etc) of the scalp in addition to the hair loss itself. These changes vary depending on the stage of presentation as well as the specific underlying cause of the alopecia.
Another clinically working approach to patients with scarring and non-scarring alopecia is to broadly group these into some sub-categories. The first is patchy alopecia, in which there is the development on the scalp of one or more variably distributed and irregularly shaped areas of alopecia. The prototype of a patchy non-scarring alopecia is alopecia areata, while the prototype of a scarring alopecia is lichen plano pilaris. The second major category that is clinically defined is pattern alopecia, in which patients present with clinically recognized pattern of hair loss such as the Ludwig classification in FPHL [ see diagram.] Other diseases, however, may also be present with patterns that may overlap what we would otherwise normally recognize as androgenetic alopecia.
Alopecia Areata (AA)
As we mentioned, Alopecia Areata is manifested by patchy areas of hair loss on the scalp and other body parts (eyebrows, eyelashes, etc) that can progress to complete loss of all body hair. It is an uncommon cause of hair loss affecting less than 2% of the population. The etiology is unknown, but autoimmune pathogenesis is suspected. AA appears to be a systemic disease because there is frequent involvement of organs other than the hair follicles in question. A complete medical history and physical exam including scalp biopsies may be necessary for the appropriate diagnosis and treatment.
Telogen Effluvium (Hair Shedding)
Telogen Effluvium is characterized by a perturbation of the hair growth cycle resulting in abnormally high shedding rate of hairs in the telogen or resting phase. The reason for such hair loss requires full examination of the patient’s history including lab tests. e.g., endocrine, nutritional or autoimmune status, hair pull test and perhaps also scalp biopsies. More than 25% of telogen hairs are diagnostic of telogen effluvium.
There are several causes of telogen effluvium:
• Drugs
-Prescribed medications
-Over the counter
• Pregnancy
• Diet- protein calorie restriction, iron, zinc or biotin deficiency. Crash diets.
• Psychological stress- high fever, chronic illness,
• Hormonal- hypothyroidism, post-menopausal
• Post-surgical
• Emotional stress
• Liver or renal failure
After the cause of the hair loss is identified and treated appropriately, the hair will regrow over a period of 6-12 months, occasionally longer due to the severity of the loss. If the cause is not found the disease can become chronic.
Cicatricial (Scarring Alopecia)
Cicatricial hair loss is typically associated with changes of the skin of the scalp. In this section we include several diseases such as: pseudopelade of Brocq, lichen plano, lichen plano pilaris, systemic lupus, sarcoidosis, scleroderma, dermatomyositis, etc. A complete medical history, lab tests and scalp biopsies for the hair specialist are critical for the appropriate diagnosis and treatment. Most of the patients with this type of diseases may require medical and topical treatment and not be candidates for hair transplant surgery.
Hair-Shaft Abnormality
Hair shaft abnormalities include several diseases that require the appropriate evaluation, diagnostic and treatment by the specialist.
Congenital
The possible causes are aplasia cutis congenital (bald spot in the crown) or triangular or patchy alopecia in temple or other areas of the scalp. The patient could be good candidate for hair transplant surgery.
Trichotillomania (Hair Pulling Tic or Mania)
This is an obsessive-compulsive disorder that consists of the hair pulling tic or mania. The patient plucks his own hair and will require psychological evaluation and treatment before a hair restoration procedure could be considered.
Trauma
Car accidents, burns (chemical or thermal), wounds, trauma or traction in the scalp can produce destruction of the hair follicles with alopecia and scarring areas of the scalp that may require different surgical treatment options such as scalp tissue expansion and/or hair transplant surgery.

Cancer
Lesions in the scalp, primarily caused by skin cancer metastasis from other site, can also produce damage to hair follicles and alopecia. The specialist must evaluate the patient for proper diagnosis and treatment.
Radiation
Exposure to ionizing radiation for the treatment of cancer of the head or scalp can result in temporary side effect and may take up to 6-12 or more months for the hair to regrowth or permanent alopecia, depending on the total dosage administered. If the hair loss is permanent the patient could be a good candidate for hair transplant surgery.

Chemotherapy
Chemotherapy (drugs for cancer) damages not only cancer cells but also healthy cells. Some chemotherapy drugs can damage the hair follicles and can produce hair loss. When hair loss occurs it is a temporary side effect and may take up to 6-12 or more months for the hair to regrow after the drug treatment has been terminated.
Infection
Fungal, bacterial and viral scalp infections may also cause hair loss and scarring
Diagnosis
As we mentioned above, women with FPHL will vary from 40-60% of all the cases. For that reason it is critically important that the evaluation should be performed by an experienced hair loss and hair restoration surgeon specialist. The evaluation should include a discussion of personal and family history, general exam, scalp evaluation and hair analysis. Lab tests and scalp biopsies may also be required.
Treatment Options
Hundreds of hair loss treatments (both homeopathic and medical) can be found over the counter, on the internet, through friends and family recommendations, newspaper, magazines, etc. Unfortunately the reality is that most of these “miracle therapies” are expensive and lack scientific evidence about what they are promoting. Without the scientific research they lose credibility and in many cases contain ingredients that do not work to combat the primary causes of hair loss.
There are medical and non-surgical options. However hair transplant surgery is the only permanent hair solution for hair loss – we will discuss this topic in the procedures section.
The best treatment for each female patient will depend of the cause of hair loss. Currently, it has been eviewed hair loss scientific studies and approved for the treatment of FPHL the following:
• Topical 2% and 5% minoxidil for women with thinning hair and hair loss.
• Low-level laser therapy for the treatment of thinning hair.
• Spironolactone- oral
Each of these treatments has different mechanisms of action and several studies have shown that the combination of treatments has better results than one single treatment. The main goals of these treatments are to slow hair loss and in some individuals to re-grow previously thinning hair. However, sustained use of these products is necessary to prevent more hair loss or even for maintenance of existing hair. If you cease using these treatments, the results will diminish and the hair loss will resume.
Clinical studies of Finasteride 1 mg (oral medication) involving post-menopausical women with FPHL didn’t show statistical improvement. The use of Finasteride has shown efficacy in female hyperandrogenism and hair loss.
Antiandrogen therapies including the androgen receptor blockers spironolactone, cyproterone acetate, and flutamide as well as oral contraceptives are used actively in Europe.
Hair Systems, Wigs, and Scalp Topical Powder.
In some cases the hair systems or wigs, particle powder, sprays could be the best cosmetic treatment.
At Spain Hair Transplantation, we will evaluate your case and advise you the best treatment options available.
Conclusion
Female pattern hair loss (Androgenetic Alopecia) is the most common hair loss condition in women with 40-60% of all the cases. The onset, rate, and severity of hair loss is unpredictable. The pathogenesis of FPHL involves genetic and hormonal components and can be inherited from either or both parents. Ludwig classification has three characteristics patterns of hair loss for the evaluation of FPHL. Appropriate diagnosis of your hair loss by an experienced hair restoration doctor is critical for choosing the best treatment options.
At Spain Hair Transplantation we are happy to help you to customize a medical and/or surgical plan especially for you to achieve your personal and professional goals. Please contact us for an appointment for the evaluation.