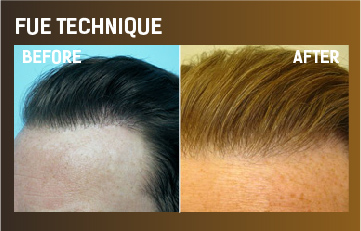
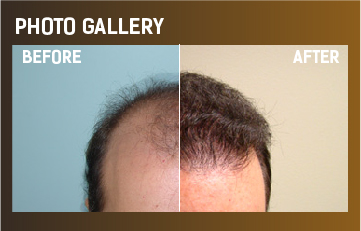
Each hair in the human scalp is unique and has a normal hair growth cycle. While hair growth cycle dynamics vary somewhat between different mammalian species, and their location on the body, there are systemic and local factors that can modulate the hair follicle activity. The scalp hair growth cycle includes three phases: growth or anagen (2 to 8 years). The second phase, catagen (2-3 weeks) is transitional. The third phase is the resting (telogen) or shedding phase that lasts 3 to 4 months. This hair cycle is asynchronous. The scalp hair follicles are 86-89% in growth phase, 1% in transitional phase and 10-13% in the shedding phase. The hair growth rate is 0.3-0.5 mm/day or 1.0 – 1.5 cms/month. Generally speaking we lose between 50-150 hairs everyday, in most of the cases the hair regrows because of the healthy hair follicle.

In MPHL there is a progressive shrinkage of the follicles, which produces an ever-diminishing amount of hair. The growth phase is increasingly shortened resulting in shorter hairs, while the percentage of hairs in the resting phase increases. Hair literally thins as one ages. Normally, the hair diameter reaches its peak between 25-30 years of age, then loses approximately 5% of diameter between 30-50 years old and 15% between 50-70 years of age. The hair shafts in male pattern baldness become progressively smaller in diameter and length. Eventually the hair produced by the declining follicle is fragile and will fall out. In men with male pattern baldness, all the hair in an affected area may eventually become involved in the process and overtime the scalp region will be covered with furry filament not unlike that of the newborn baby. Hair pigment production also decreases and terminates with miniaturization so the fine hair becomes lighter and lighter in color and may completely fall out over time.
The MPHL involves both hormonal and genetic components. Inheritance is a key factor; genes can be inherited from either parent. Some men are not affected even those who are advanced in age. Recently a possible high relative risk of balding has been found in young men if they had a balding father.
Classification for Hair Loss in Men
Norwood has classified seven different patterns of male hair loss (see illustration below). The classification is very useful and has its limitations and some patients do not fit into its categories. Although the density of hair in a given pattern of loss tends to diminish with age, there is no way to predict what pattern of hair loss a young man with early male pattern baldness will eventually assume. In general, those who begin losing hair in the early 20’s are those in whom the hair loss will be the most severe. In some men, initial male-pattern hair loss may be delayed until the late 30’s or 40’s. It is generally recognized that men in their 20’s have a 20 percent incidence of male pattern baldness, in their 30’s a 30 percent incidence of male pattern baldness, in their 40’s a 40 percent incidence of male pattern baldness and so forth. Using these numbers one can see that a male in his 90’s has a 90 percent chance of having some degree of male pattern baldness. The Norwood classification is a good reference for an organized and systemic approach (medical and/or surgical) for the hair loss patient.

Other Causes of Hair Loss in Men
Hair loss may be broadly grouped in several ways, the first of which is non-scarring vs. scarring alopecias. Clinically, non-scarring alopecias the prototype of which is androgenetic alopecia or MPHL and alopecia areata demonstrate hair loss without changes in the texture or appearance of the scalp. In general, scarring alopecias the prototype being lichen plano pilaris on the other hand typically demonstrate associated changes of the skin (redness, inflammation) of the scalp in addition to the hair loss itself. These changes vary depending on the stage of presentation as well as the specific underlying cause of the alopecia.
Another clinically working approach to patients with scarring and non-scarring alopecia is to broadly group these into some sub-categories. The first major category that is clinically defined is pattern alopecia, in which patients present what is clinically recognized pattern of hair loss such as the Norwood classification in MPHL. The second is patchy alopecia, in which there is the development on the scalp of one or more variably distributed and irregularly shaped areas of alopecia. The prototype of a patchy non-scarring alopecia is alopecia areata while the prototype of a scarring alopecia is lichen plano pilaris. Other diseases, however, may also be present with patterns that may overlap what we would otherwise normally recognize as androgenetic alopecia (genetic hair loss)
Alopecia Areata (AA)
As we mentioned, it is manifested by patchy areas of hair loss in the scalp and other body parts (eyebrows, eyelashes, etc) that can progress to complete loss of all body hair. It is a less common cause of hair loss affecting less than 2% of the population. The etiology is unknown, but autoimmune pathogenesis is suspected. AA appears to be a systemic disease because there is frequent involvement of organs other than the hair follicle. A complete medical history and physical exam including scalp biopsies may be necessary for the appropriate diagnosis and treatment.

Telogen Effluvium (Hair Shedding)
It is characterized by a perturbation of the hair growth cycle resulting in an abnormally high rate of shedding of hairs in the telogen or resting phase. The reason for such hair loss requires a full examination of the patient’s history including lab tests. e.g., endocrine, nutritional or autoimmune status, hair pull test and perhaps scalp biopsies. More than 25% of telogen hairs are diagnostic of telogen effluvium.
There are several causes associated with this process:
• Drugs
-Prescribed medications
-Over the counter medications
• Diet- protein calorie restriction, iron, zinc or biotin deficiency. Crash diets.
• Psychological stress- high fever, chronic illness
• Hormonal- hypothyroidism
• Post-surgical
• Emotional stress
• Liver or renal failure
After the cause of the hair loss is identified and treated the hair will regrow over a period of 6-12 or (more) months. If the cause is not found the disease can become chronic.
Cicatricial (scarring alopecia)
Typically demonstrate associated changes of the skin of the scalp. In this section we include several diseases such as: pseudopelade of Brocq, lichen plano, lichen plano pilaris, systemic lupus, sarcoidosis, scleroderma, dermatomyositis, etc. A complete medical history, lab tests and scalp biopsies for the hair specialist are critical for the appropriate diagnosis and treatment. Most of the patients with this type of diseases may require medical and topical treatment and aren’t candidates for hair transplant surgery until the hair loss cause is stable.
Hair-Shaft Abnormality
Hair shaft abnormality includes several diseases that require the appropriate evaluation, diagnosis and treatment by a specialist.
Congenital
The possible causes are aplasia cutis congenital (bold spot in the crown) or triangular or patchy alopecia in temple or other areas of the scalp. The patient could be a good candidate for hair transplant surgery.
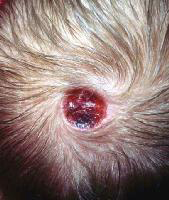
Aplasia Cutis Congenital
Trichotillomania (Hair Pulling Tic or Mania)
This is an obsessive-compulsive disorder that consists of hair pulling tic or mania. The patient plucks his own hair and will require psychological evaluation and treatment.
Trauma
Car accidents, burns (chemical or thermal), wounds, trauma or traction in the scalp can produce destruction of the hair follicles with alopecia and scarring areas of the scalp that may require different surgical treatment options including scalp tissue expansion and/or hair transplant surgery.

Cancer
Lesions in the scalp as primary skin cancer or a metastasis from another site can also produce damage to hair follicles and alopecia. The specialist must evaluate the patient for proper diagnosis and treatment.
Radiation
Exposure to ionizing radiation can result in temporary or permanent hair loss, depending on the total dosage administered. When hair loss occurs it is a temporary side effect and may take up to 6-12 or more months for the hair to regrow after the drug treatment has been terminated. If the hair loss is permanent the patient is a candidate for hair transplant surgery
Chemotherapy
Chemotherapy (drugs for cancer) can damage not only cancer cells but also healthy cells. Some chemotherapy drugs can damage the hair follicles and can produce hair loss. When hair loss occurs it is a temporary side effect and may take up to 6-12 or more months for the hair to regrow after the drug treatment has been terminated.
Infection
Fungal, bacterial and viral scalp infections may also cause hair loss and scarring.
Diagnosis
As we mentioned above, it is critical and important to have a complete evaluation of the patient with hair loss. The evaluation should include personal and family history, general exam, scalp evaluation and hair analysis. Lab tests and scalp biopsies may also be required.
Treatment Options
Hundreds of hair loss treatments and solutions (both homeopathic and medical) can be found over the counter, on the Internet, through friends and family recommendations, newspaper, magazines, etc. Unfortunately, the truth of the matter is that most of these “miracle therapies” are expensive, lack sufficient scientific research to prove their validity and safety about what they are promoting and without scientific studies they lose all credibility.
There are medical and non-surgical options. However hair transplant surgery is the permanent hair solution for hair loss, we will discuss this topic in the procedures section.
The best treatment for each patient will depend on the cause of hair loss. Currently, the USA FDA has reviewed hair loss scientific studies and approved the following treatments for MPHL:
• Minoxidil 2% and 5%, (both are topical solutions)
• Finasteride 1 mg (oral medication) and
• Low-level laser therapy The portable handheld device and the full head unit (similar to a hair dryer)
Each of these treatments functions in its own way but several studies have shown that the combination of treatments promotes better results than one single treatment. The main goals with the treatment are to slow hair loss and, in some individuals to re-grow previously thinning hair. However, sustained use of these products is necessary to prevent more hair loss or even for maintenance of existing hair; failure to do so may result in continued hair loss.
Hair-Systems and Scalp Topical Powder
In some cases a hair system or wig and topical powder could be the non-surgical or non-medical options based on the severity of the loss or the nature of the specific type of hair loss.
At Spain Hair Transplantation, we will evaluate your case and advise you of the best treatment options available if you want to make the transition from a wig to hair transplant surgery.
Conclusion
Male pattern hair loss is by far the most common condition in men. The onset rate and severity of hair loss is unpredictable. The origins of MPHL involve genetic and hormonal components and can be inherited from either or both parents. The Norwood classification has several characteristic patterns of hair loss for the evaluation of MPHL. Appropriate diagnosis of your hair loss by an experienced hair restoration specialist is critical for choosing the best treatment options available in each case. Please contact us for your consultation and evaluation.